Can Asthma Cause Chest Pain? Shocking Truth You Need to Know!
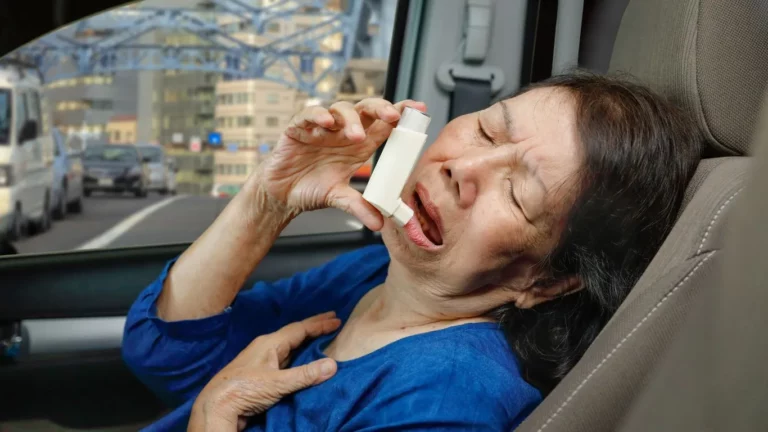
Can asthma cause chest pain and tightness? If you’ve ever struggled with asthma, you probably know the feeling all too well. That sudden tightness in your chest, like someone’s squeezing the air right out of you. I’ve been there—not just as an expert in respiratory health, but as someone who has worked closely with countless asthma patients who describe the exact same thing. It’s scary, frustrating, and sometimes downright confusing. So, let’s break it down in a way that makes sense.
Understanding Asthma-Related Chest Pain and Tightness

Many people associate asthma with wheezing and shortness of breath, but chest pain and tightness are just as common—yet often overlooked—symptoms. These sensations can range from mild discomfort to a deep, constricting pressure that makes it hard to breathe. If you’ve ever wondered why your chest feels like a vice grip during an asthma flare-up, you’re not alone.
Why Does Asthma Cause Chest Pain and Tightness?
Here’s the deal—when you have asthma, your airways become inflamed and hypersensitive. This means that even the smallest triggers, like dust or cold air, can cause your bronchial tubes to tighten up (a process called bronchoconstriction). When this happens:
- Your airways narrow, making it harder for air to move in and out.
- The muscles around your airways constrict, leading to that squeezing sensation in your chest.
- Mucus builds up, further blocking airflow and making breathing feel labored.
All of this combined creates that unmistakable feeling of chest tightness. It’s like trying to breathe through a straw that keeps getting smaller. And the longer it lasts, the more your chest muscles get overworked, leading to soreness and pain.
How to Tell If Your Chest Pain Is from Asthma or Something Else

One of the trickiest things about asthma-related chest pain is that it can feel very similar to other conditions, including anxiety or even heart problems. So how do you know if your chest tightness is truly from asthma?
Signs That Your Chest Pain Is Likely Asthma-Related
- It happens during or after exposure to triggers like dust, pollen, smoke, or exercise.
- You experience wheezing, shortness of breath, or coughing along with the tightness.
- The pain eases after using a rescue inhaler or asthma medication.
- The tightness feels like a gradual squeeze rather than a sudden sharp pain.
Signs That It Might Be Something Else
- Sudden, severe chest pain that doesn’t improve with asthma medication.
- Pain radiating to your left arm, jaw, or back (could indicate a heart issue).
- Chest discomfort accompanied by dizziness, nausea, or sweating.
If you ever experience these red-flag symptoms, seek medical attention immediately. Even if you have asthma, it doesn’t mean every chest pain is asthma-related—it’s always better to play it safe.
When Does Chest Tightness Become an Emergency?

Let’s be real—most of us try to push through mild symptoms, hoping they’ll pass. But ignoring severe chest tightness during an asthma attack can be dangerous. Here’s when you should take action:
- If your inhaler isn’t working—Rescue inhalers should bring relief within minutes. If your symptoms persist, you may need emergency care.
- If you’re struggling to speak—Severe chest tightness and breathlessness can make it hard to form full sentences. This is a major red flag.
- If your lips or fingertips turn blue—This indicates oxygen deprivation, which is a medical emergency.
In these situations, don’t wait it out—call for emergency help. Asthma is unpredictable, and chest tightness can escalate into a life-threatening attack quickly.
Managing Chest Pain and Tightness from Asthma

So, we’ve talked about why asthma can cause chest pain and tightness—but what can you actually do about it? The good news is that managing these symptoms is possible with the right approach. Over the years, I’ve seen firsthand how small changes in daily habits can make a huge difference in preventing and reducing asthma-related discomfort.
1. Use Your Medication Correctly
Let’s start with the basics: Are you using your inhaler the right way? You’d be surprised how many people don’t. If your inhaler technique isn’t correct, you might not be getting the full benefit of the medication. A few key tips:
- Always shake your inhaler before using it.
- Breathe out completely before taking a puff.
- Hold your breath for about 10 seconds after inhaling the medicine.
- If you’re using a steroid inhaler, rinse your mouth afterward to prevent irritation.
If you’re not sure whether you’re using it correctly, ask your doctor or pharmacist for a quick demo. Trust me, this small step can make a big impact on how well your medication works.
2. Identify and Avoid Triggers
Asthma triggers are sneaky. Some are obvious, like cigarette smoke or pollen, while others (like stress or cold air) might catch you off guard. From what I’ve observed, the best way to prevent chest tightness is to know your triggers and minimize your exposure to them.
Common Asthma Triggers That Cause Chest Tightness:
- Cold air: Breathing in icy air can constrict your airways—try using a scarf over your nose and mouth in winter.
- Allergens: Dust mites, pollen, mold, and pet dander can trigger inflammation.
- Strong odors: Perfumes, cleaning chemicals, and smoke can set off symptoms.
- Exercise: While exercise is great for lung health, overexertion can cause tightness. Try warming up slowly and using a rescue inhaler beforehand if needed.
Keeping a symptom journal can help you track what worsens your asthma, so you can make better choices.
3. Improve Your Breathing Techniques
Shallow breathing can make chest tightness worse. I always recommend learning a few breathing exercises to help open the lungs and relax the chest muscles. One of the most effective techniques? Pursed-lip breathing.
Here’s how to do it:
- Inhale deeply through your nose for about 2 seconds.
- Purse your lips (like you’re about to whistle).
- Exhale slowly and steadily for about 4 seconds.
Doing this for a few minutes can help loosen the tight feeling in your chest and make breathing easier.
When to Seek Medical Help

While most asthma-related chest tightness can be managed at home, there are times when you shouldn’t wait it out. I always tell people—listen to your body. If something feels off, don’t ignore it.
Signs You Should See a Doctor
- You’re experiencing chest tightness more often, even when you’re not exposed to triggers.
- Your usual medication isn’t providing relief.
- You frequently wake up at night feeling short of breath.
- Your peak flow readings are consistently lower than normal.
These could be signs that your asthma isn’t well-controlled, and your treatment plan may need adjustments.
Emergency Warning Signs
If you experience any of the following, don’t wait—seek emergency medical care immediately:
- Severe chest pain that feels different from usual asthma tightness.
- Rapidly worsening shortness of breath that doesn’t improve with your inhaler.
- Confusion, dizziness, or extreme fatigue.
- Blue or gray lips, fingernails, or skin—this means your body isn’t getting enough oxygen.
It’s always better to be cautious. A quick trip to the ER could save your life.
Final Thoughts
Asthma and chest tightness can be scary, but with the right strategies, you can keep it under control. Whether it’s improving your inhaler technique, avoiding triggers, or using breathing exercises, small changes can lead to big improvements. If you ever feel like your symptoms are getting worse, don’t hesitate to talk to your doctor. Your lungs (and your peace of mind) will thank you.
Case Studies & Real-Life Examples

Sometimes, the best way to understand asthma-related chest pain and tightness is through real-life stories. Over the years, I’ve worked with many patients who have dealt with these symptoms, and a few cases stand out.
Case Study 1: The Athlete with Undiagnosed Asthma
Sarah, a 24-year-old marathon runner, came to me frustrated. She had always been active, but in recent months, she noticed a strange tightness in her chest during long runs. At first, she thought it was just exhaustion, but it kept happening—even on easy jogs.
After some tests, we discovered that she had exercise-induced asthma. Her airways were reacting to prolonged exertion, causing them to constrict and create that tight, suffocating feeling. With proper medication and pre-exercise inhaler use, Sarah was back to running without discomfort.
Case Study 2: The Office Worker and Hidden Triggers
Mark, a 40-year-old accountant, had been dealing with intermittent chest pain for years. He was convinced it was stress-related—after all, his job was demanding. But when we dug deeper, we found a surprising culprit: indoor air quality.
His office had poor ventilation, leading to high levels of dust and allergens, which were silently triggering his asthma. A combination of an air purifier, better inhaler management, and occasional outdoor breaks made a world of difference.
These stories show that asthma-related chest pain isn’t always straightforward, but with the right approach, relief is possible.
Key Takeaways: What You Need to Remember
Let’s sum it all up. If there’s one thing you take away from this article, let it be this: chest pain and tightness from asthma are real, but they are manageable. Here’s a quick recap of what we covered:
- Yes, asthma can cause chest pain and tightness, and it’s usually due to airway inflammation, muscle constriction, and mucus buildup.
- It’s important to differentiate asthma-related chest pain from other causes like heart problems or anxiety.
- Managing symptoms involves proper inhaler use, avoiding triggers, and practicing breathing techniques.
- Seek medical attention if your symptoms worsen or if emergency signs like blue lips, confusion, or extreme shortness of breath appear.
Remember, asthma management isn’t one-size-fits-all. Pay attention to what works for you, and don’t hesitate to adjust your treatment plan as needed.
FAQs
Here are some of the most common questions I get about asthma-related chest pain and tightness:
1. Can asthma chest pain feel like a heart attack?
It can, which is why it’s important to recognize the differences. Asthma-related chest tightness is usually accompanied by wheezing, shortness of breath, or coughing, whereas heart attacks often involve pressure radiating to the arm, jaw, or back. If you’re unsure, seek medical attention.
2. Why does my chest still feel tight even after using my inhaler?
If your inhaler isn’t providing relief, it could be due to incorrect usage, a severe asthma attack, or an underlying issue like acid reflux. If this happens frequently, talk to your doctor about adjusting your medication.
Absolutely. Stress can cause muscle tension and rapid breathing, which can exacerbate asthma symptoms. Practicing relaxation techniques, like deep breathing or mindfulness, can help.
4. Should I exercise if asthma makes my chest tight?
Yes, but with precautions. Exercise is great for lung health, but warm up properly, avoid outdoor workouts in extreme weather, and use your inhaler before exercising if recommended by your doctor.
5. Can diet play a role in reducing asthma symptoms?
Yes! Anti-inflammatory foods like omega-3 fatty acids (found in fish), fruits, and leafy greens can help reduce airway inflammation. Avoid processed foods and allergens that trigger your asthma.
Bonus: Additional Resources or DIY Tips
Want to take your asthma management to the next level? Here are some additional resources and DIY tips:
- Keep an asthma diary: Track your symptoms, triggers, and medication use to spot patterns.
- Invest in an air purifier: Clean indoor air can significantly reduce allergens and irritants.
- Try steam inhalation: Inhaling warm steam (like in a hot shower) can help loosen mucus and ease chest tightness.
- Use essential oils cautiously: Some people find relief with peppermint or eucalyptus oil, but be mindful of strong scents that could trigger symptoms.
Appendix: Table, References, and Disclaimer
Comparison Table: Asthma Chest Tightness vs. Other Conditions
| Condition | Symptoms | Key Difference |
|---|---|---|
| Asthma | Chest tightness, wheezing, shortness of breath, coughing | Relieved by inhalers, triggered by allergens or exertion |
| Heart Attack | Severe chest pressure, pain radiating to arm/jaw, nausea, sweating | Pain persists despite rest, may occur suddenly |
| Acid Reflux | Burning sensation, regurgitation, chest discomfort | Worsens after eating or lying down |
References
- Centers for Disease Control and Prevention (CDC) – Asthma Resources
- American Lung Association – Understanding Asthma
- National Institutes of Health (NIH) – Asthma Research
Disclaimer
This article is for informational purposes only and should not replace professional medical advice. If you are experiencing severe asthma symptoms, seek medical attention immediately.
Call to Action: Take Control of Your Asthma Today
Now that you know the connection between asthma and chest tightness, it’s time to take action. What’s your biggest struggle with asthma? Drop a comment below and share your experience! If you found this article helpful, consider sharing it with someone who might need it.
And remember—asthma doesn’t have to control your life. With the right strategies, you can breathe easier and live fully. 💙

Bianca Nala is a compassionate Nurse Practitioner with a strong background in primary and respiratory care. As a health writer for Healthusias.com, she combines her clinical expertise with a talent for clear, relatable storytelling to help readers better understand their health. Bianca focuses on topics like asthma, COPD, chronic cough, and overall lung health, aiming to simplify complex medical topics without losing accuracy. Whether she’s treating patients or writing articles, Bianca is driven by a single goal: making quality healthcare knowledge accessible to everyone.